Can Automation Improve Imaging Center Scalability? Explained
Imaging centers juggle a steady flow of patients, machines and data with little margin for error. Automation offers the prospect of smoother throughput by shifting routine tasks away from humans so clinicians can focus on judgment and patient contact.
Many stakeholders weigh promises against costs and culture, asking if machines will truly help the center grow without eroding quality. The real answer hangs on how systems are chosen, how staff are prepared and how work is rearranged to match new capabilities.
The Scalability Challenge For Imaging Centers
Imaging centers often face surges in demand that expose fragile parts of their operation, from registration counters to reading rooms. Bottlenecks show up as delayed appointments, idle scanners and rushed reports that can slow growth and frustrate both staff and patients.
Scaling up is not just about buying more hardware but about making daily routines repeatable and predictable so capacity can stretch without chaos. A pragmatic look at workflows reveals where a bit of automation can turn a bottleneck into a reliable step.
How Automation Streamlines Patient Intake
Patient intake includes a number of small steps that add up to significant time and variation when handled manually. Automated pre registration, digital forms and identity checks can cut wait times and reduce data entry errors while letting front desk staff focus on complex questions.
When intake systems feed directly into scheduling and imaging orders, the chain from arrival to scan tightens and becomes easier to manage.
Many centers see this as the first step toward a workflow where imaging operations move faster and staff can focus more on patient care than paperwork. That said, good design keeps the human touch in place for patients who prefer a person at key moments.
Scheduling And Resource Allocation With Automation
Good scheduling must juggle machine time, technologist availability and patient needs in a way that feels fair and efficient. Automated scheduling tools can suggest optimal slots, balance load across scanners and flag gaps that might be filled to avoid wasted time.
Smart rules reduce last minute cram sessions and help centers add more exams without hiring at the same pace, which is often the path to true scale. Still, rules have to be tuned, and staff should be able to override suggestions when real world circumstances call for judgment.
Image Acquisition And Protocol Consistency
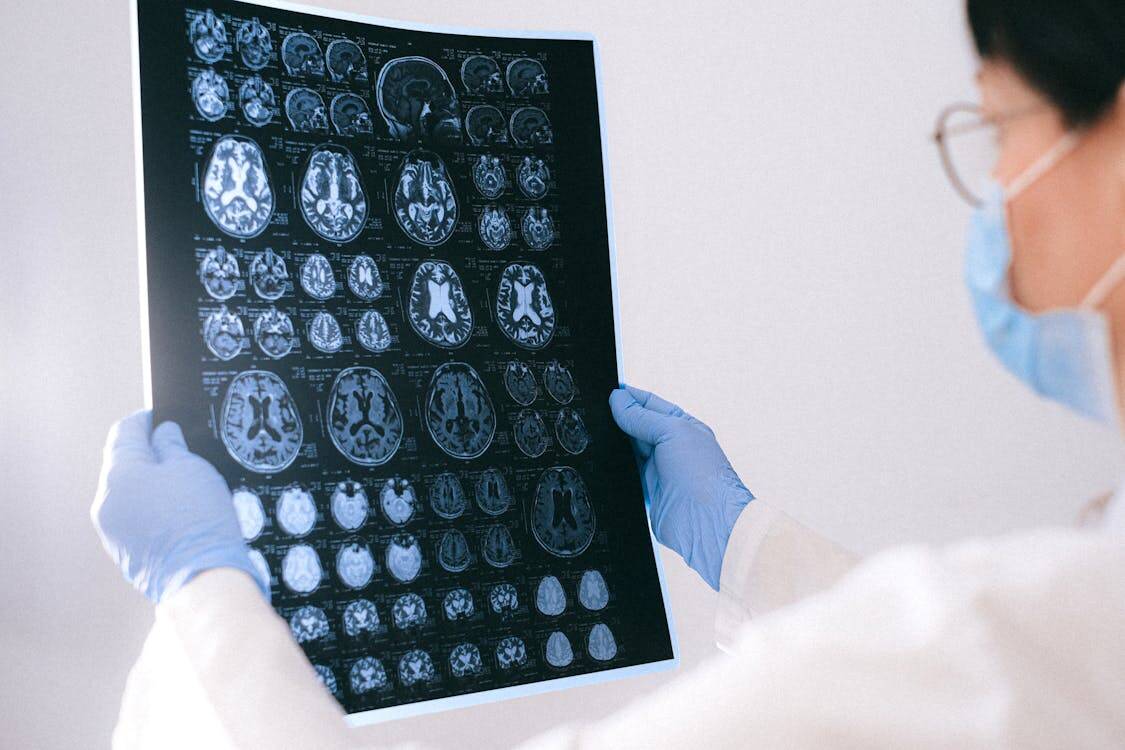
Consistency in how scans are performed matters for both diagnostic quality and throughput predictability. Protocol automation can standardize parameter selection so similar exams look alike across technologists and shifts, which helps radiologists read faster and trust their comparisons.
Automation also reduces the odds of repeat scans that happen because a setting was missed or a field of view was wrong, saving time and lowering patient exposure to imaging. That kind of consistency supports scaling by turning variation into repeatable steps that stack neatly through the day.
Workflow Integration And Interoperability
Automation is only as strong as the connections it creates between systems, from electronic health records to picture archiving tools and billing platforms. When systems share data smoothly, fewer manual handoffs are required and the whole process from order to report moves with fewer interruptions.
Integration reduces duplication of effort and the kinds of errors that slow growth, while providing a clearer picture of where to invest next. Building those bridges takes careful attention to standards, testing and a willingness to refine interfaces after they go live.
Quality Control And Error Reduction
Automation can act like a second pair of eyes, flagging anomalies that might escape busy staff whether those are mismatched study labels or unexpected changes in image quality.
Automated quality checks run consistently and do not tire, catching patterns that suggest equipment drift or training gaps long before a human auditor would spot them.
Reducing errors has a ripple effect: fewer callbacks, faster reads and stronger patient trust all help a center serve more people effectively. Of course, automation catches many issues but not every nuance, so human oversight remains part of the loop.
Staff Roles And Job Design
When machines take on routine tasks the day to day work of staff shifts and new roles emerge that call for different skills. Technologists may spend more time on patient interaction and complex setups while supervisors concentrate on exceptions and continuous improvement.
Thoughtful job redesign helps avoid the common pitfall where new tools are piled on top of existing responsibilities, creating stress rather than relief. Engaging staff in the change process reduces friction and helps leaders spot unintended consequences quickly.
Cost Implications And Return On Investment
The financial picture of automation is not a simple purchase equation but a forecast that includes time saved, error reduction and capacity to accept more cases. Upfront costs cover software, integration and training while recurring expenses include maintenance and support contracts that must be budgeted.
Centers that measure throughput, repeat rates and staff time before and after deployment have a clearer story to tell about return on investment and can make smarter choices about where to scale next. If the numbers line up, modest automation investments can open the door to meaningful growth without linear increases in payroll.
Data Management And Reporting
As centers scale the volume of images and reports grows rapidly and the need for timely analytics becomes pressing. Automated reporting tools can assemble operational dashboards that reveal idle scanner time, average patient wait and report turnaround in ways that humans cannot track easily by memory.
Better data supports decisions about where to expand hours, which technicians need more training and whether to add a second scanner. Careful attention to data governance keeps reports honest and helps leaders trust the numbers that guide expansion.
Adoption Hurdles And Change Management
Even well chosen technology can fail to deliver when people feel left out or when old habits quietly persist beneath a new veneer of automation. Clear communication, phased rollouts and training that matches real tasks help teams move from skepticism to steady adoption.
Leaders who collect feedback and adjust workflows after launch find the system more resilient and useful than those who treat rollout as a one time event. Patience matters; cultural shifts take time and small course corrections often lead to better long term outcomes.




